DIGITAL INTERACTIVE SERVICES
Fire Digital Transformation by FHIR
Today, healthcare organizations are being challenged by a multitude of factors. There is a growing need for seamless data flow between different operating systems and a sharper focus on data quality, security, and efficiency. The sector is yet to achieve this goal of data-enabled health systems. Thanks to the current digital upheaval and some favourable mandates by the Center for Medicare and Medicaid Services (CMS), Fast Healthcare Interoperability Resources (FHIR®) has helped in making this coveted data interchange a reality.
Driving modernization to comply with FHIR mandates could undoubtedly create opportunities to redefine the patient and provider experience. However, a pre-requisite for this potential opportunity is to go beyond the absolute minimum ask and kick-start modernization across the healthcare landscape. This will pave the way to a true digitally-connected healthcare system that provides seamless end-to-end patient care, whilst improving overall health outcomes.
Healthcare Interoperability and FHIR
As the healthcare sector evolved, several attempts were made at creating an ideal healthcare interoperability standard. The intent was to improve and strengthen connections across various systems to support the exchange of clinical documents. What started in the 1980s finally saw a frontrunner in 2014, with the developer-friendly HL 7 FHIR standard which enabled true interoperability between systems.
FHIR is an API-focused (application programming interface) standard used to exchange essential health information. FHIR is maintained by Health Level 7 (HL7®), the standards development organization enabling safe data transfer between various health care providers. Simply put, FHIR is a common set of schema, definitions, and APIs with a higher standard for global health data interoperability that is working towards handling the increasing demand. However, FHIR could not have attained its present commercial viability if it was not for the push by CMS.
CMS’s path towards a Connected Healthcare System
The adoption of FHIR-based API standards for data interoperability is being strongly encouraged by CMS, and for specific criteria, it is mandated. CMS requires FHIR-based regulations to facilitate patient-centred care and promote informed decision-making. As a result, the adoption of the HL7 FHIR standard has become more crucial than ever to satisfy regulatory requirements, and other strategic demands, among service providers and payers.
In addition to defining the data exchange policies, CMS offers several plug-ins for FHIR-based APIs that allow healthcare systems to link and access Medicare and Medicaid data without altering the current legacy systems. For instance, the Beneficiary Claims Data API when linked with FHIR APIs enables access to bulk data files, the Blue Button 2.0 FHIR APIs allow its users to retrieve vital Medicare beneficiary information, and so on.
The adoption of FHIR in the current healthcare systems
According to a study by Change Healthcare in 2021, 24% of US healthcare stakeholders presently utilize FHIR APIs but 90% of them believe that FHIR will be widely used by 2024 as it is essential for the future of healthcare. Organizations around the world are capitalizing on FHIR adoption as a springboard toward modernization to start their digital transformation journey. That said, healthcare systems will need to invest more effort, and perhaps overcome some integration challenges, to fully embrace this change.
The stepping stone to embracing this change
FHIR was introduced in 2014 and the CMS FHIR mandates came into existence in 2019. A substantial percentage of legacy systems developed before this were not FHIR compliant, and so these may face challenges in it being renewed as per FHIR. Legacy systems will have numerous tactical and operational questions, such as whether to build a new system from scratch, buy something commercially off-the-shelf, customise only the required modules, or rehost the cloud for compliant APIs. A further debate could arise due to key criteria like the modernisation cost, complexity, market value, and time required to take the final output to market.
One efficient way to upgrade legacy systems is to extend them without disrupting or replacing the existing flow. Incorporating an FHIR extension could be the ideal solution.
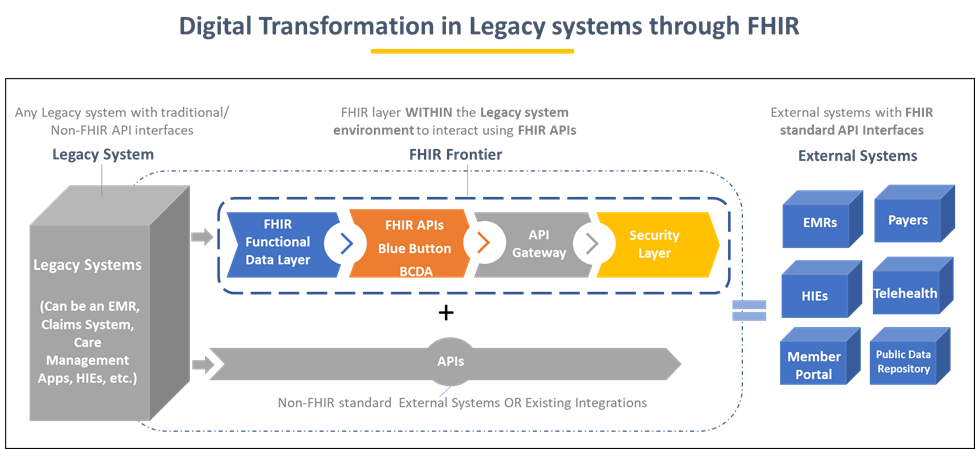
FHIR extensions, a plug-and-play FHIR frontier, connect the legacy systems and the external world by communicating through FHIR-APIs. FHIR extensions can be scaled depending on the demand. For example, these extensions can be scaled to support CMS’s APIs such as Blue Button 2.0, BCDA APIs, Data at Point of Care APIs, etc. to access medicare beneficiary data, if required.
In the post-pandemic world, we know only too well what a boon it would be to have all our medical data available online across various medical operating systems. Maybe that future is not too far away after all.






